
Structured Interdisciplinary Bedside Rounds (SIBR) on an acute care medical unit
Well Begun is Half Done
MONTH
Physician & staff engagement, unit co-leads

MONTH
Training, custom tools, and Day 1


MONTH
03
Daily data, skills certification, and leadership dashboards

Results Speak Louder than Words
Awards are the Echoes of Excellence
One Key, Many Doors
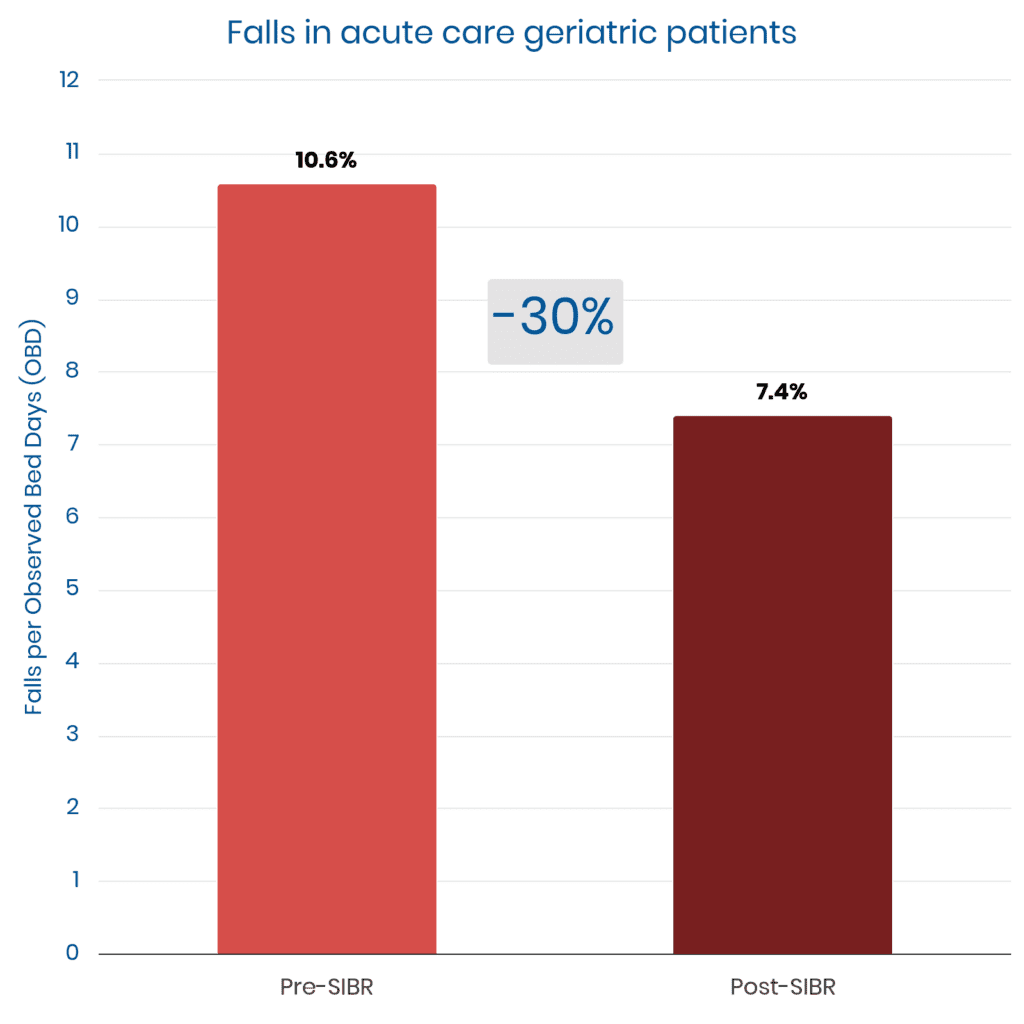

SIBR teams review quality-safety checklists together at the bedside daily, typically addressing 10+ known risks of hospitalization.
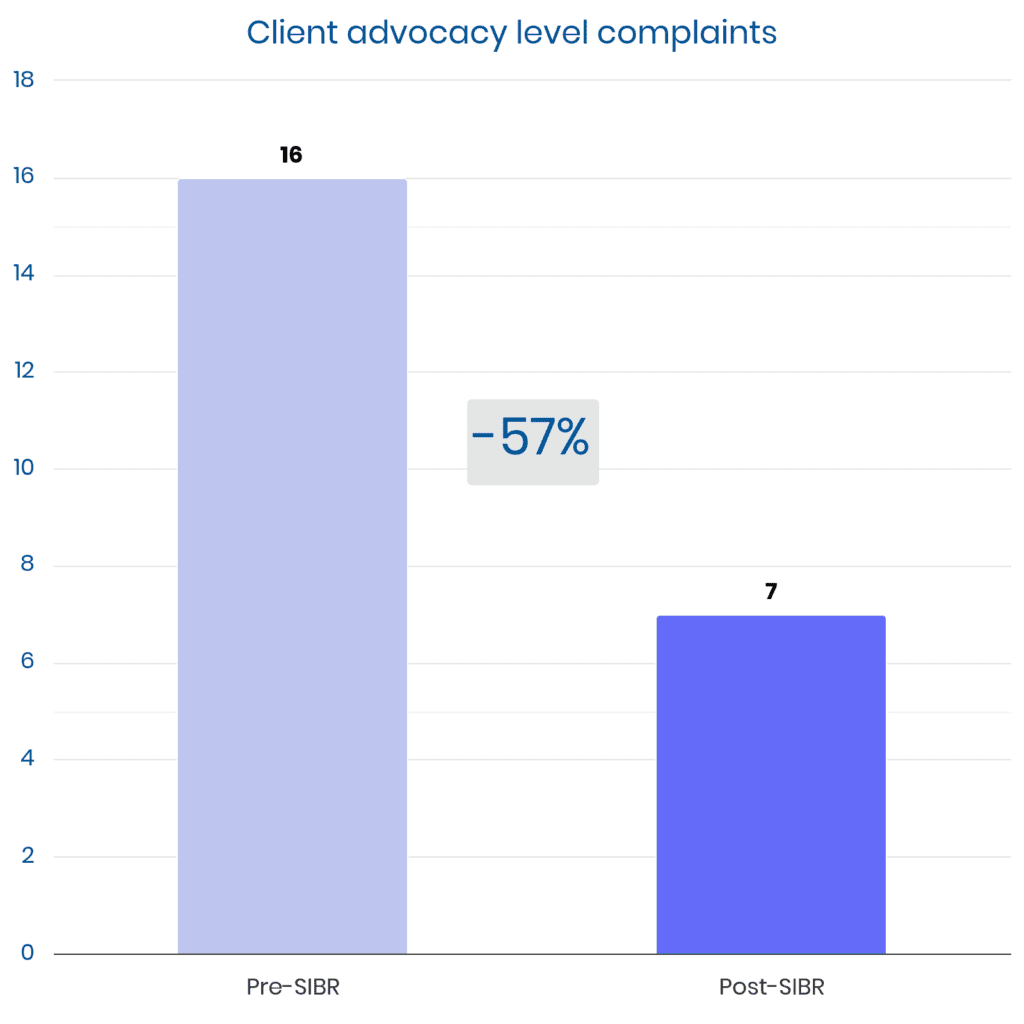

SIBR Rounds encourage family participation, proactively answer common questions and provide a dedicated time to hear from the care team.
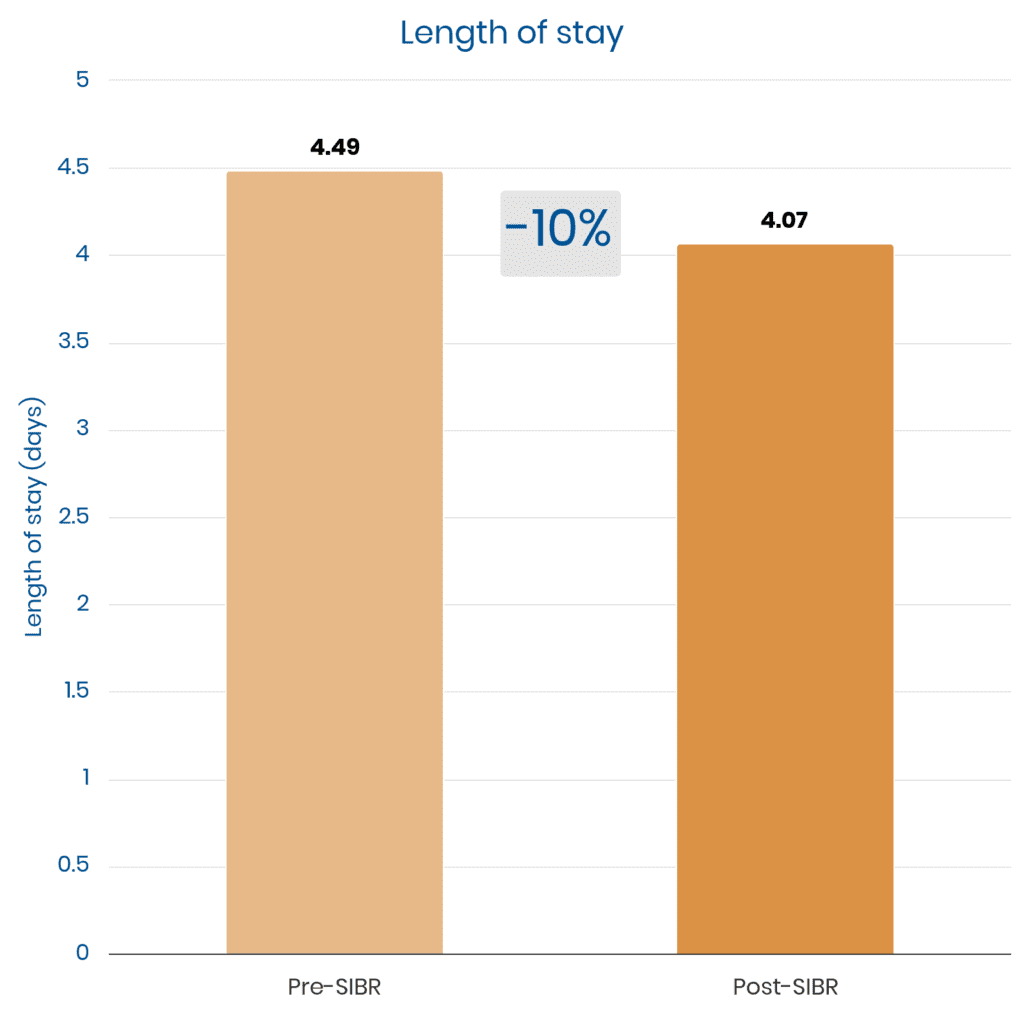

SIBR Rounds hardwire the ideal discharge huddle, ensuring physicians and care managers always give an EDD and include the patient, family, and bedside nurse in transition planning.
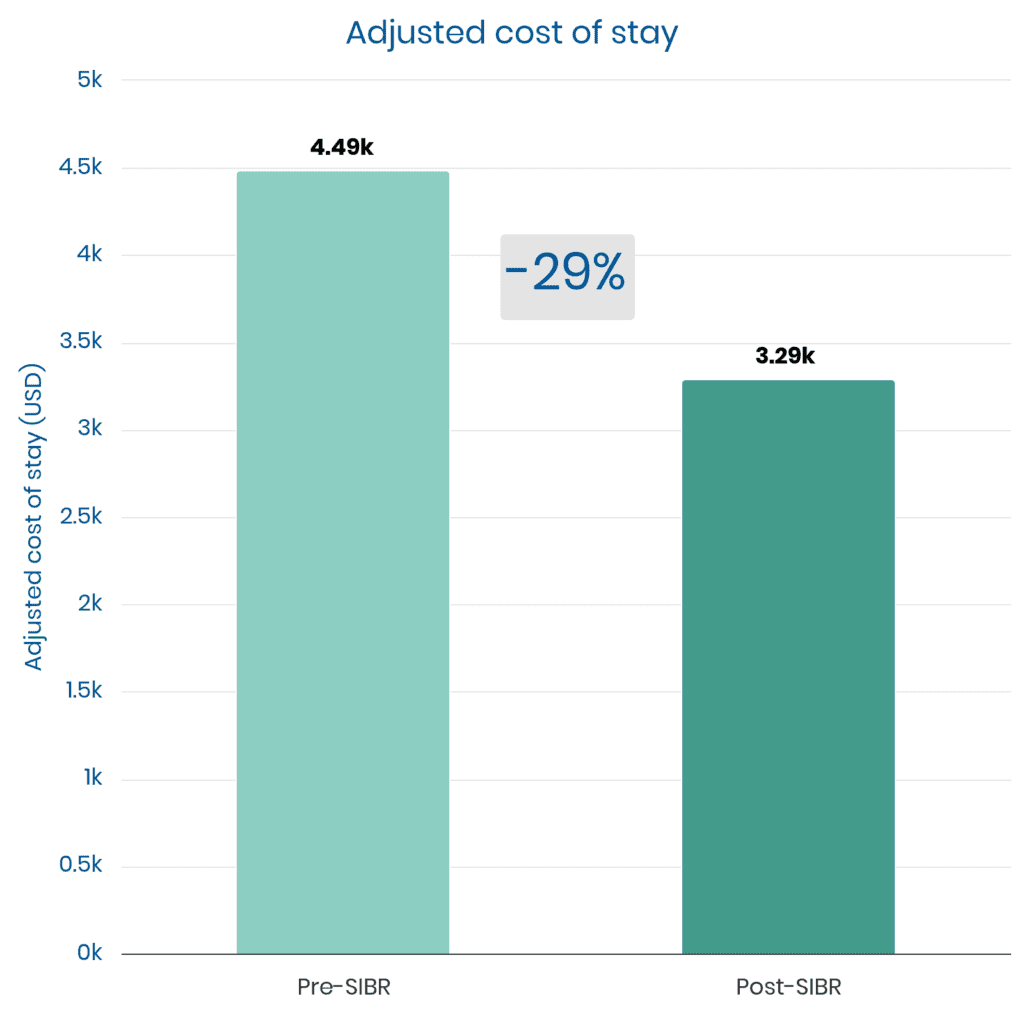

SIBR Rounds prevent waste and by improving care and reducing inefficiencies, saving millions each year.
A structured Bedside Shift Report and Change of Shift Huddle that most nurses prefer, hardwired using field-tested tools and training.
The award-winning, evidence-based gold standard of acute care teamwork – Structured Interdisciplinary Bedside Rounds.
















Credentialed Credibility
What next?
Seeing is Believing
Knowledge is Power
The Wise Learn from the Wise
© 2024 • 1Unit • All rights Reserved.